AAPC recommends these 5 steps:
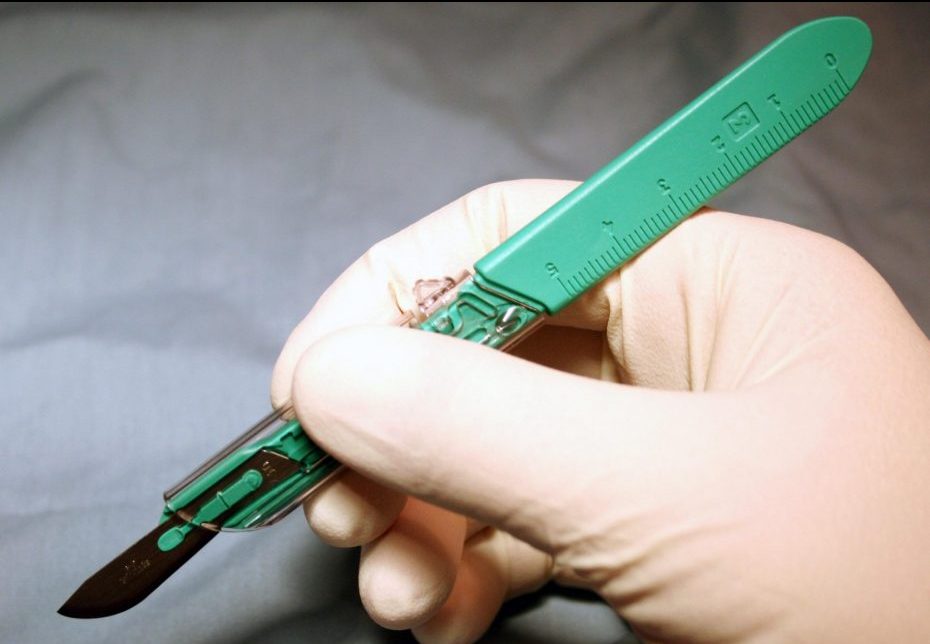
Step 1: Measure First, Cut Second
Step 2: Wait for the Pathology Report
Step 3: Location Matters
Step 4: Bundle Simple Repairs with Excision
Step 5: Report Each Lesion Separately
 www.aapc.com
www.aapc.com
Under certain circumstances, it may be necessary to indicate that a procedure or service was distinct or independent from other non-E/M services performed on the same day. Modifier 59 is used to identify procedures/services, other than E/M services, that are not normally reported together, but are appropriate under the circumstances. Documentation must support a different session, different procedure or surgery, different site or organ system, separate incision/excision, separate lesion, or separate injury (or area of injury in extensive injuries) not ordinarily encountered or performed on the same day by the same individual. However, when another already established modifier is appropriate it should be used rather than modifier 59. Only if no more descriptive modifier is available, and the use of modifier 59 best explains the circumstances, should modifier 59 be used.
Modifier 51 impacts payment. ... While modifier 51 and 59 both apply to additional procedures performed on the same date of service as the primary procedure, modifier 51 differs from modifier 59 in that it applies to procedures that may be more commonly expected to be performed during the same session.
Modifier 51 Multiple procedures indicates that the same provider performed multiple procedures—other than E/M services—at the same session. You should list the most resource-intense (highest paying) procedure first and append modifier 51 to the second and subsequent procedures.
Use modifier 51 to indicate:
 www.cms.gov
www.cms.gov
Modifier 59 Distinct procedural service is used to indicate a:
A few additional resources:

 www.aafp.org
www.aafp.org

 ohiohima.blogspot.com
ohiohima.blogspot.com

 www.icd10monitor.com
www.icd10monitor.com
CCO free wound care resource.
This free Wound Measurement & Repair Grid serves as the perfect ‘cheatsheet’ for medical coders.
If you’re trying to figure out the correct medical codes for wound repair, then this grid will help out immensely.
Fill out the information on the right to request it instantly.
Wound Measurement and Repair: Click Here to Download
The physician removed a lesion from the patient’s nose along the supra-alar crease. The lesion measures at 1.5 cm at its widest point and there was an allowance of 1.0 cm margin on all sides. The pathology report later confirmed that the lesion was benign.
To calculate, consider the narrowest margin (1.0 cm) x 2 = 2 cm. Add this figure to the widest measurement of the lesion (1.5 cm) for a 3.5 cm total. Based on the location of the lesion (nose) and the total measurement (3.5 cm), the correct code is 11444 Excision, other benign lesion including margins, except skin tag (unless listed elsewhere), face, ears, eyelids, nose, lips, mucous membrane; excised diameter 3.1 to 4.0 cm.

 www.aapc.com
www.aapc.com
Coding Guidelines
 www.cms.gov
www.cms.gov
Step 1: Measure First, Cut Second
Step 2: Wait for the Pathology Report
Step 3: Location Matters
Step 4: Bundle Simple Repairs with Excision
Step 5: Report Each Lesion Separately

Lesion Excision: 5 Steps to Coding Success
When assigning codes for lesion excision, you must know the size of the lesion(s) and the width of the margins (the area around the lesion also removed).
Under certain circumstances, it may be necessary to indicate that a procedure or service was distinct or independent from other non-E/M services performed on the same day. Modifier 59 is used to identify procedures/services, other than E/M services, that are not normally reported together, but are appropriate under the circumstances. Documentation must support a different session, different procedure or surgery, different site or organ system, separate incision/excision, separate lesion, or separate injury (or area of injury in extensive injuries) not ordinarily encountered or performed on the same day by the same individual. However, when another already established modifier is appropriate it should be used rather than modifier 59. Only if no more descriptive modifier is available, and the use of modifier 59 best explains the circumstances, should modifier 59 be used.
Modifier 51 impacts payment. ... While modifier 51 and 59 both apply to additional procedures performed on the same date of service as the primary procedure, modifier 51 differs from modifier 59 in that it applies to procedures that may be more commonly expected to be performed during the same session.
Modifier 51 Multiple procedures indicates that the same provider performed multiple procedures—other than E/M services—at the same session. You should list the most resource-intense (highest paying) procedure first and append modifier 51 to the second and subsequent procedures.
Use modifier 51 to indicate:
- Same procedure, different sites
- Multiple operation(s), same operative session
- Procedure performed multiple times
Proper Use of Modifier 51 | CMS
Providers and their billing representatives must use caution when using modifier 51. It is inappropriate to use multiple procedure modifiers when there is no second procedure performed.
Modifier 59 Distinct procedural service is used to indicate a:
- Different session or encounter
- Different procedure
- Different site
- Separate incision, excision, lesion, injury, or body part
A few additional resources:
https://downloads.cms.gov/medicare-coverage-database/lcd_attachments/35498_13/L35498_DERM011_BCG.pdf

12 Errors to Avoid in Coding Skin Procedures
Coding and billing for diagnosing and treating skin lesions is rife with potential pitfalls that could lead to delayed payments at best and increased insurer scrutiny or investigation for fraud at worst. Because skin procedure codes take into account the type of removal, the size and location of...

Coding the Excision of Lesions
This edition of “Spotlight on CPT” is going to explore the proper coding for excision of lesions. First, coding professionals must be...

2019 CPT® Coding for Skin Biopsies
Skin biopsy codes are changing. EDITOR’S NOTE: This is an updated version of the second installment in a two-part series on the 2019 CPT® codes released
CCO free wound care resource.
This free Wound Measurement & Repair Grid serves as the perfect ‘cheatsheet’ for medical coders.
If you’re trying to figure out the correct medical codes for wound repair, then this grid will help out immensely.
Fill out the information on the right to request it instantly.
Wound Measurement and Repair: Click Here to Download
The physician removed a lesion from the patient’s nose along the supra-alar crease. The lesion measures at 1.5 cm at its widest point and there was an allowance of 1.0 cm margin on all sides. The pathology report later confirmed that the lesion was benign.
To calculate, consider the narrowest margin (1.0 cm) x 2 = 2 cm. Add this figure to the widest measurement of the lesion (1.5 cm) for a 3.5 cm total. Based on the location of the lesion (nose) and the total measurement (3.5 cm), the correct code is 11444 Excision, other benign lesion including margins, except skin tag (unless listed elsewhere), face, ears, eyelids, nose, lips, mucous membrane; excised diameter 3.1 to 4.0 cm.

Skin Lesion Measuring Tips
CPT® provides different code sets to report excision of benign (11400-11471) and malignant (11600-11646) skin lesions/neoplasms. The codes within each set

Coding Guidelines
- For excision of benign lesions requiring more than simple closure, i.e., requiring intermediate or complex closure, report 11400-11466 in addition to appropriate intermediate (12031-12057) or complex closure (13100-13153) codes. For reconstructive closure, see 14000-14300, 15000-15261, and 15570-15770.
- CPT codes 11400-11446 should be used when the excision is a full-thickness (through the dermis) removal of a lesion, including margins, and includes simple (non-layered) closure.
- Excision is defined as full-thickness (through the dermis) removal of a lesion, including margins, and includes simple (non-layered) closure when performed. Each benign lesion excised should be reported separately.
- Code selection is determined by measuring the greatest clinical diameter of the apparent lesion plus that margin required for complete excision (lesion diameter plus the most narrow margins required equals the excised diameter). The margins refer to the most narrow margin required to adequately excise the lesion, based on the physician's judgment. The measurement of lesion plus margin is made prior to excision.
MCD Search
The Redesigned MCD Search Page lets you search on a keyword, code, or document ID



